Ankle Pain and Instability
Ankle instability
Ankle instability is experienced either as:
- a lack of trust in the ankle (ie a sense that the ankle could give way at any time)
- the ankle actually giving way (which may lead to a fall)
Some people experience this instability whilst walking on flat ground, whilst others may require a higher force for such as changing directions in netball or stepping into a pothole
Instability may be the result of single high force injury (such as landing on an uneven ground from a significant height) or from, multiple lower energy events (ankle sprain during a casual jog around the park)
Anatomy
The ankle is made up of:
- 3 bones (Tibia/Talus/Fibula)
- 3 ligaments (Lateral/Medial/Syndesmosis). Each ligament has multiple components.
Causes
The most common cause of ankle instability is an inversion / plantarflexion event results in injury to the anterior talofibular ligament.
There are also many intra-articular causes. Intra-articular implies within the joint itself, rather than from the ligaments surrounding the ankle joint.
Intra-articular causes of instability include
- loose bodies that can become entrapped within the ankle joint
- avulsion fractures (when a small chunk of bone attached to a tendon or ligament gets pulled away from the main part of the bone)
- osteochondral defects of the talar dome (where the smooth cartilage surface that allows the ankle to glide has crater-like chunks of cartilage missing)
- impingement or blocking of the ankle joint by an overgrowth of scar tissue following an injury.
Symptoms
- The ankle movement may feel restricted, especially in the upwards movement (dorsiflexion)
- The ankle may feel generally unstable
- Recurrent ankle sprains
- Pain at the front or the back of the ankle made worse when squatting
- Crepitus in the ankle joint, otherwise known as clicking, crunching or grinding in the joint.
What Imaging is Needed?
Depending on the suspected injury, mechanism of injury and physical examination, there are multiple imaging options that your healthcare professional may choose to use.
The first choice of imaging is usually weight-bearing x-rays taken at 3 different angles. If an x-ray does not give enough detail, other imaging modalities may be used.
- An Ultrasound will be able to identify ligament injuries.
- A CT scan will be able to identify fractures, loose bodies that may be within the joint space or any bony spurs.
- An MRI scan will identify an osteochondral defect may be present on the articular surface of the talus. An MRI scan will also be able to identify if a syndesmosis injury is present.
Non-Surgical Treatment
The identification of a ligament tear in diagnostic imaging does not always mean surgery is required. Quite often, your surgeon will refer you to allied health, such as physiotherapy or podiatry, because the ligament tear can successfully be treated without surgery. This can include the use of strengthening programs, proprioception training and the use of ankle braces for stability.
ATFL ligament injuries are usually only referred for surgery when non-surgical treatment has failed, in other words if ankle sprains continue despite a committed attempt at rehabilitation, or if the obvious cause of pain or instability cannot be treated by a non-surgical means. This will be discussed at your consultation with the surgeon.
Medial ligament injuries and Syndesmosis injuries (High ankle sprain) are usually more complex and require further discussion with your surgeon.
Surgical Treatment
The aim of surgery is to stabilize the ankle joint.
The main option for surgical treatment of ankle instability is Lateral Ligament Reconstruction.
Ligament reconstruction
This operation is often performed in conjunction with an ankle arthroscopy.
It requires an incision along the outside of the ankle joint.
The ligament is then reconstructed using your own ligament tissue and sutures.
If you are hypermobile (“double jointed”), the ligament will be reinforced with a surgical tape.
This procedure will require at least 2 weeks of complete non-weightbearing whilst wearing a CAM-boot.
Once the wound has healed, early range of motion physiotherapy can begin. During the early stages of rehabilitation, there is to be no inversion or eversion. You will remain in the CAM-Boot or the ASO sfor 6 weeks but remove the boot for non-weightbearing range of motion exercises. At 7 weeks post-operatively, intensive physiotherapy will begin. The overall recovery time for a ligament reconstruction varies from 3-6 months.
Rehabilitation Plan
Our team will walk you through your rehabilitation program after surgery. This table is a guide and changes may be required depending on your progress.
LATERAL LIGAMENT RECONSTRUCTION
On your mobile? Click the green + to see the full instructions for each week
| Week | Exercises | Boot | Weight bearing | Returning to Pre-Surgical Function | Other |
|---|---|---|---|---|---|
| 0-2 | Toe wriggling Hip, knee AROM exercises. | Cast | Non weight bearing | Staying home with the foot elevated above heart level for 23 hours a day | |
| 2-4 | Once wounds healed, begin passive ROM exercises. Hip, knee band resisted exercises. Toe lifts, bends, pulls, pushes. | Cam boot | Weight bear as tolerated | ||
| 4-6 | Seated CRs, feet tapping, short foot and arch lift exercises. Continue exercises a/a. Physio guided ankle mobilisations. Begin gently ankle circles without resistance | Cam boot/ASO brace | Weight bear as tolerated | Return to work – sedentary occupation. | |
| 6-8 | Start DL heel raises, progressing to SL. Physio guided resisted ankle eversion and inversion. | ASO brace | Full weight bearing | Return to light duties – labour intensive occupation | |
| 8-10** | Physio guided gait and balance training. | May return to full duties | |||
| 10-12* | Physio guided, gradual return to pre-surgery activities eg. running, cycling. | ||||
| 12+ | Return to sport training if criteria met and physio clinical assessment passed. | VAS pain score of <5/10 during and after exercise. Resolving joint effusion. DF ROM within 10% of opposite side. Y balance test within 6cm of opposite side. Hop test within 90% of opposite side. |
If you have any questions please do not hesitate to contact Mr Goldbloom’s rooms on 03 9650 0534.
This rehabilitation plan was developed by Mr Goldbloom in conjunction with Physiotherapists Brodie Leonard-Shannon and Brendan Mason from Back in Motion, Aspendale Gardens.
Cartilage injury of the ankle
The ankle joint is covered by a smooth substance called “hyaline cartilage”. This allows the ankle to glide easily between “dorsiflexion” and “plantarflexion”. Hyaline cartilage is vulnerable to damage from:
- sprains and fractures around the ankle
- deficiency of the underlying subchondral bone.
The term “osteochondral defect” (OCD) is often applied in such cases.
OCD injuries can result in:
- giving way (or an anticipation of giving way)
- locking of the ankle joint
- catching (the ankle locks fleetingly)
- grinding
- pain that is often difficult to precisely locate
These injuries are often seen on MRI and CT scans.
Surgery in the form of ankle arthroscopy +/- microfracture may be recommended to manage this problem.
Ankle Arthroscopy +/- Microfracture
During an arthroscopy, the surgeon will make two small incisions on the front of your ankle.
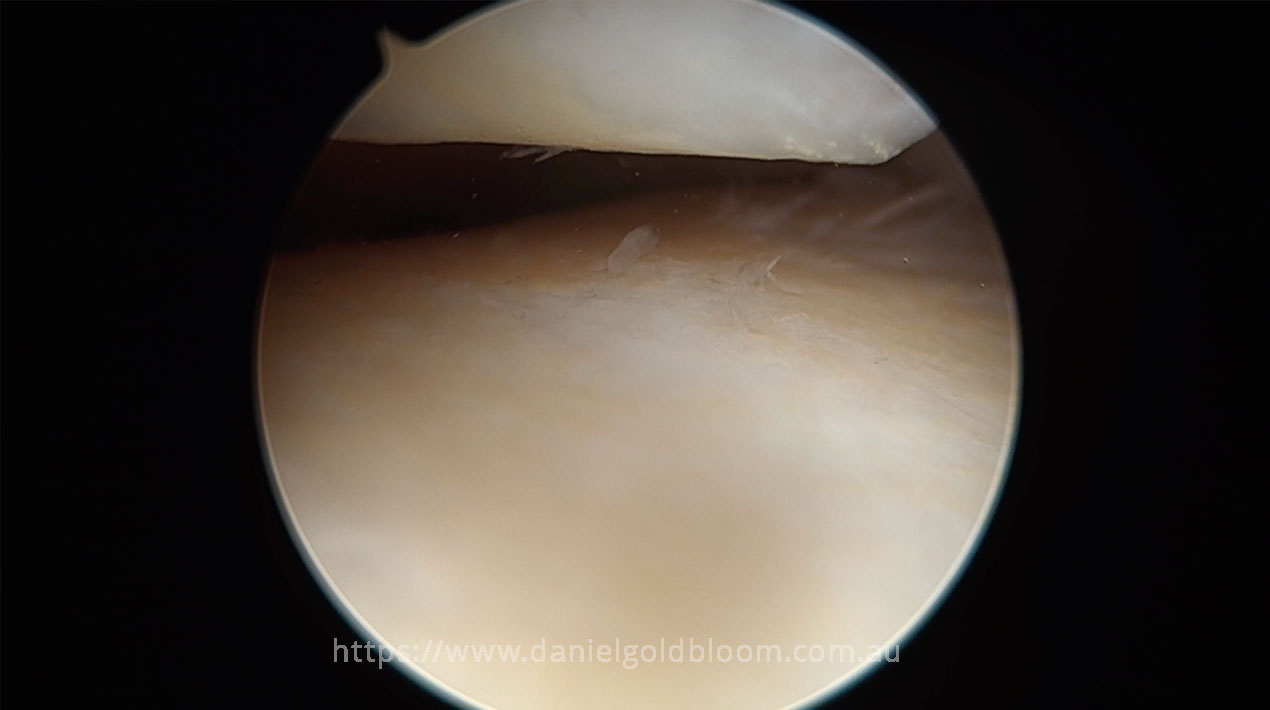
A camera will be inserted into one of the incision holes and will be used to provide a “real time examination” of the joint.
This type of surgery allows for:
- loose bodies to be removed from the joints
- removal of excessive scar tissue
- debridement (cleaning out) of inflamed joint tissue
- video assessment of the stability of the ankle joint.
- Assessment of the cartilage in the ankle, in particular the talar dome. The dome shape is very important for the smooth motion of the ankle joint. If the dome is found to have any small crater-like pieces of cartilage missing, the dome can be repaired by a number of different techniques such as microfracture. This will help to restore the normal convex cartilage surface of the talar dome.
Following this procedure, you will be fitted with a CAM-Boot but must remain completely non-weightbearing for the first 3 days. After 3 days, you will be able to weight bear as tolerated but only for essential activities such as using the bathroom. You must aim to elevate the foot for 23 hours a day above the level of your heart for the first 2 weeks in order to reduce the risk of long term swelling.
At the two-week mark, you will have a follow up appointment where the stitches will be removed. Once the wounds are fully healed, intensive physiotherapy can begin. You will continue to wear the CAM-Boot for a further 2-4 weeks and weightbear as tolerated. Around this period, you will either transition to footwear coupled with an ASO-style brace for extra support and then eventually, just into regular footwear.
The overall recovery time ranges from 4-8 weeks.
The information provided here is for general educational purposes only. Please contact Mr Goldbloom's rooms to discuss if surgery is appropriate for your situation.