Big Toe Arthritis & Joint Pain Treatment Melbourne
Big Toe Arthritis (or Hallux Rigidus) is a common condition where normal cartilage is worn away at the 1st metatarso-phalangeal joint (MTPJ) or “big toe joint“. The joint loses its normal shape, and underlying bone is exposed. There may also be formation of bony spurs (or osteophytes) around the joint. When this occurs, big toe arthritis treatment may be necessary.
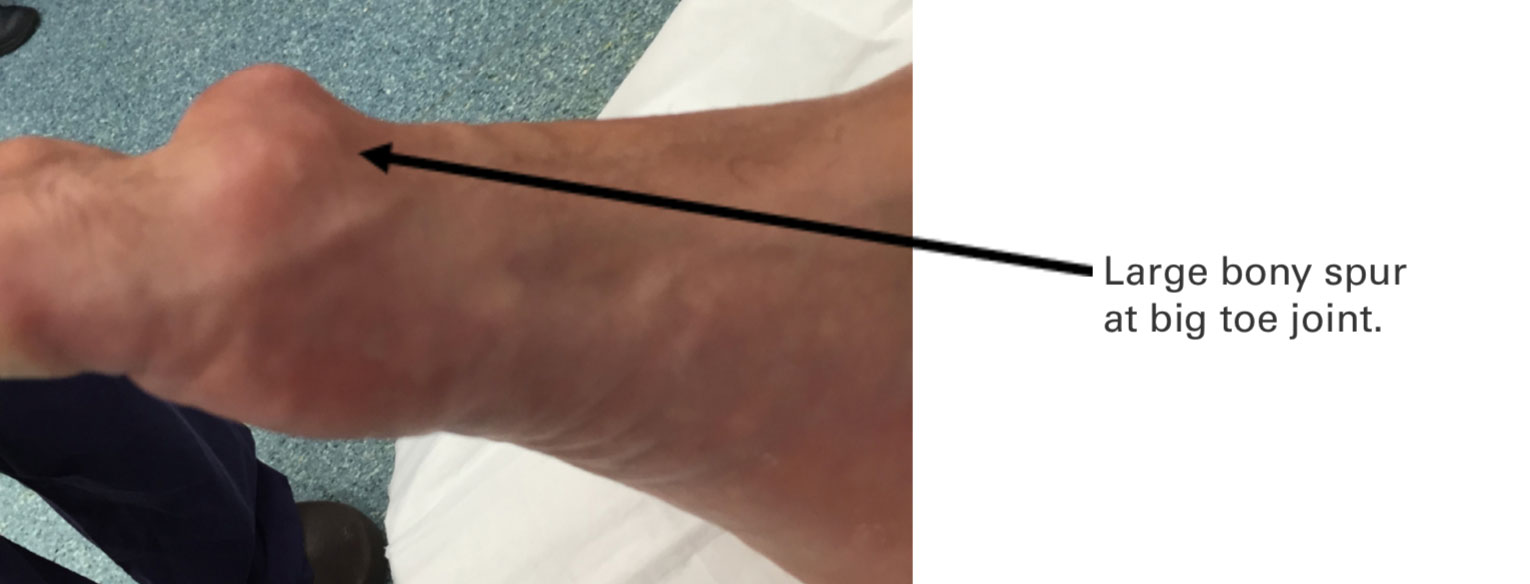
In this episode of PodMD, experienced orthopaedic surgeon Dr Daniel Goldbloom will be discussing the topic of great toe arthritis, including what great toe arthritis is, the required imaging, the expectations for surgery, the role of podiatry in this condition and more.
Causes
Hallux Rigidus is usually the result of long term “wear and tear” associated with your daily activities. It can also be related to a previous injury (post traumatic) or may be part of another condition such as gout, long standing bunions, previous infection or inflammatory diseases such as Rheumatoid Arthritis.
Symptoms
Patients experience pain and stiffness at the MTPJ of the big toe. Patients may notice a bump on the top of the joint that can rub against tight fitting shoes.
What Imaging is Needed?
‘Standing’ x-rays must be obtained to accurately assess severity of the Big Toe Arthritis. In the earlier stages, it may only be evident on Magnetic Resonance Imaging (MRI) scan.
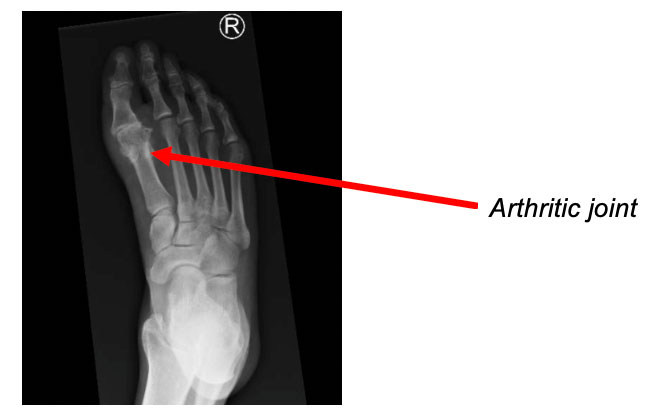
Non-Surgical Treatment
The main aim of nonsurgical treatment for Hallux Rigidus is to relieve pain by reducing the load through the arthritic joint.
A visit to the Orthotist or Podiatrist might be useful. They should be able to provide you with advice about wearing appropriate shoes and the use walking aids. In addition, they can provide a special shoe or insole that reduces movement at the painful joint.
Lifestyle and activity modifications such as weight loss and low impact exercises may help.
Pain killers prescribed by your Doctor can assist in reducing pain. Lastly, a cortisone injection may offer relief of inflammation.
Big Toe Arthritis Surgery
The aim of surgery is to walk normally without pain and to return to most regular activities of daily living.
Mr Goldbloom performs three type of surgeries for Hallux Rigidus (Big Toe Arthritis Surgery). It is important to take time at your consultation to discuss these in order to choose which is option is right for you.
Cheilectomy is a procedure that involves removal of bone on the top of the joint. This can help restore “dorsiflexion” movement (elevation of the big toe). Removing the bump also reduces the pressure from tighter fitting shoes.
Interposition Arthroplasty is a newer surgical option that involves placement of a “spacer” in the joint as well as removing the bump on the top. It treats the “bone on bone” arthritis while maintaining movement in the big toe.
Fusion or MTPJ Arthrodesis is one of the most successful procedures performed by Mr Goldbloom and is often referred to as ‘the gold standard’ for this condition. During this procedure, the remaining cartilage is removed and the joint is deliberately stiffened. Following this procedure, many patients are able to get back running. The main limitation of 1st MTP fusion is the inability to wear heels higher than 1 inch.
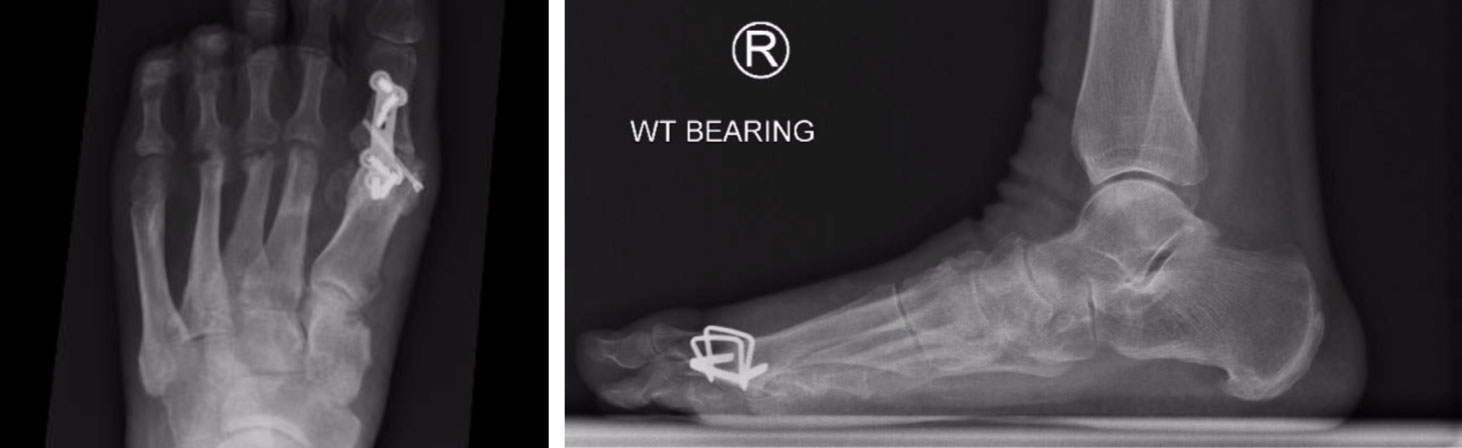
Post-operative Care
- When you go home it is very important to elevate the foot 23 hours a day above the level of your heart for two weeks.
- You will have an appointment 1-2 weeks after your operation with Mr Goldbloom and a Wound Nurse Specialist. Your dressings are to stay dry and intact until this appointment.
- Physiotherapy will be required post-operatively. It will be tailored to the type of surgery performed and how well you are recovering.
- Patients usually weight-bear in a stiff sole open toe shoe from day one for between 2-8 weeks. You will be seen by a Physiotherapist whilst in hospital who will provide you with the appropriate footwear and ensure you are able to manage your post-operative weight-bearing instructions.
Refer to the Foot and Ankle Surgery information sheet for further post-operative instructions.
Rehab Protocol for 1st MPJ Arthrodesis
On your mobile? Click the green + to see the full instructions for each week
| Week | Exercises | Boot | Weight bearing | Returning to Pre-Surgical Function | Other |
|---|---|---|---|---|---|
| 0-2 | Toe wriggling Ankle circles Foot massage | Darco | WBAT (should be sitting at home 23 hours though) | Staying home with the foot elevated above heart level for 23 hours a day | |
| 2-4 | Calf stretching. Hip, knee, ankle band resisted exercises. Toe lifts, bends, pulls, pushes. | Darco | WBAT | Return to work – sedentary occupation. | Start physio guided rehab |
| 4-6 | Seated CRs, feet tapping, short foot and arch lift exercises. Continue exercises a/a. Start DL heel raises, progressing to SL. | X-ray at 6/52 to assess FW suitability | WBAT | Walking as tolerated. Return to light duties – labour intensive occupation | |
| 6-8 | 1st toe flex and ext mobilisations, toe ball squeeze, toe squeeze and spread. Physio guided gait and balance training | Nil | WBAT | ||
| 8-10** | Increase walking distance. | Nil | FWB | May return to full duties (clinical assessment required) | |
| 10-12* | Physio guided, gradual return to pre-surgery activities eg. running, cycling. | Nil | FWB | ||
| 12+ | Return to sport training | Return to sport |
Physiotherapists aim to perform a gait assessment for patients after 6 months when their supinatory defensive gait should be gone, although this is not compulsory.
The information provided here is for general educational purposes only. Please contact Mr Goldbloom's rooms to discuss if surgery is appropriate for your situation.
