Bunion Surgery Melbourne

Watch what's involved in keyhole bunion rehab.
Produced in collaboration with the Australian Ballet.
A Bunion (or Hallux Valgus) appears as a bump on the side of the great toe. It is due to an angular deformity at the 1st MTP joint (at the base of the great toe). As a result, the great toe then pushes against the second toe. Bunions often occur in both feet and women make up the majority of cases. Bunions can occur at any age and tend to worsen over time. Keyhole bunion surgery is often a preferred way to treat this issue.
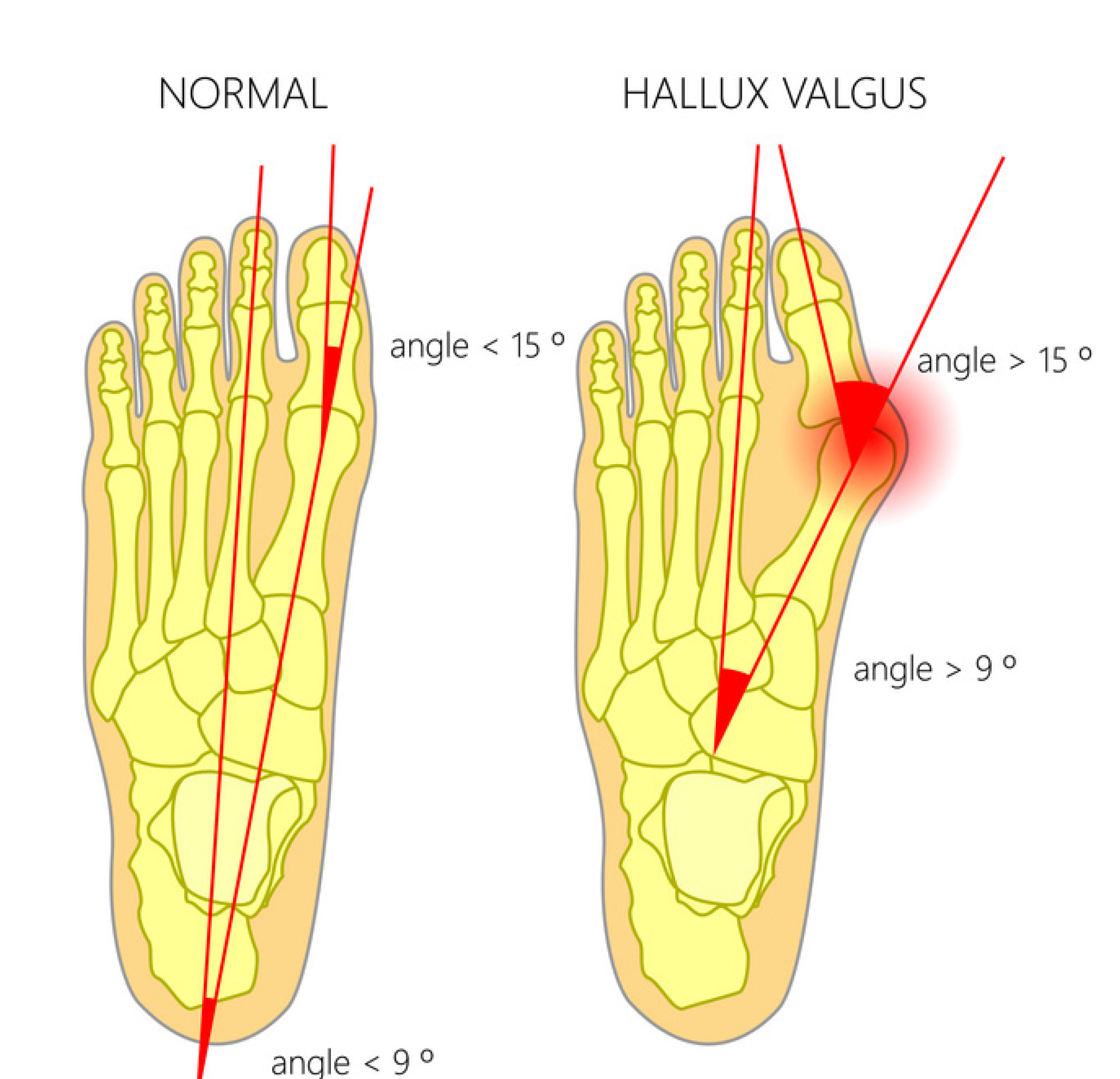
Causes
Bunions are thought to occur due to an imbalance between your ligaments and muscles in the foot. It is partly an inherited condition but footwear such as tight or high heeled shoes also contribute.
Symptoms
Patients may experience painful rubbing over the Bunion causing difficulty finding comfortable footwear or pain elsewhere in the foot. In rare cases, it can lead to a skin breakdown over the Bunion. A Bunion will often lead to issues around the second toe being painful and deformed (claw or hammer toe).
When to consider having a discussion with a Surgeon for your Bunions:
- Pain over the bunion itself
- Pain through the ball of the foot or in the big toe joint
- Worsening or concern over the appearance
- Difficulty with footwear
- Development of 2nd toe clawing
- Development of stiffness in big toe joint
- Numbness around the area.
What Imaging is Needed?
Plain ‘weight-bearing’ x-rays must be obtained to accurately assess the deformity.
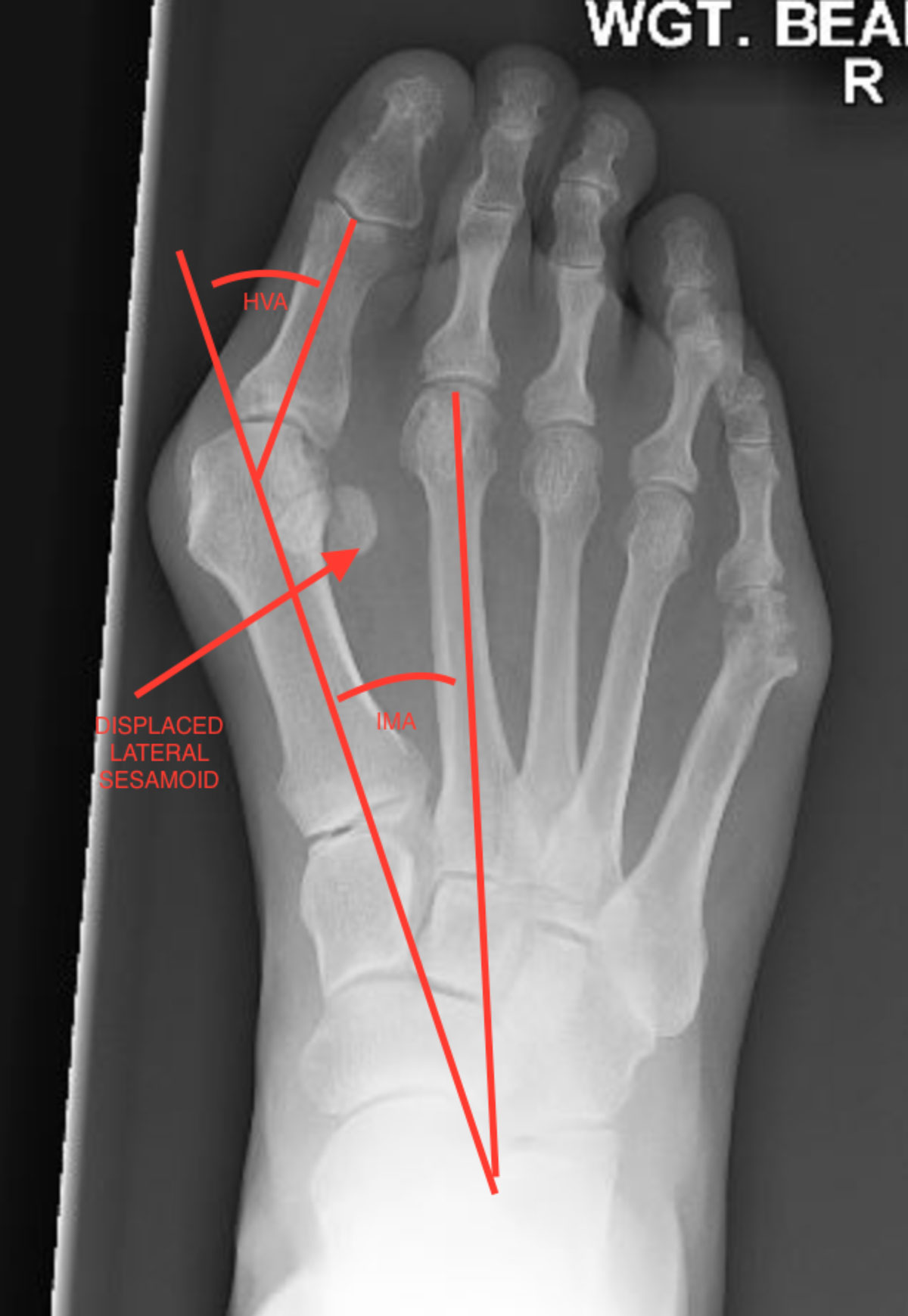
Non-Surgical Treatment
There is no non-surgical treatment that can permanently correct the deformity or prevent it getting worse. Wider shoes can accommodate the foot and limit rubbing. An Orthotist or Podiatrist should be able to provide you with a Bunion splint to hold the toe in a corrected position.
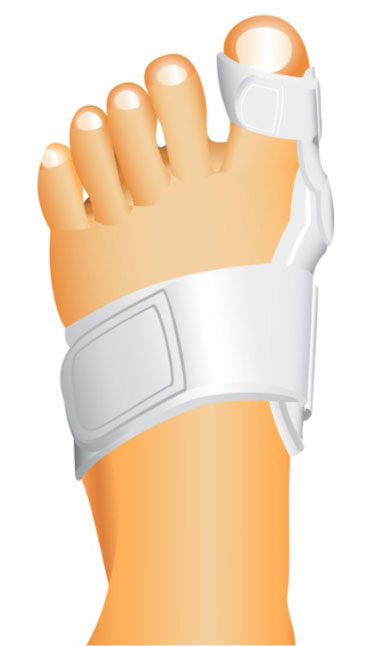
Bunionectomy Surgery
Surgical treatment is the most reliable way to correct your bunion. Most patients achieve a successful outcome after bunion surgery.
Mr Goldbloom is an experienced surgeon, focusing on delivering expert bunionectomy surgery for patients. He prefers minimally invasive surgery for Bunion correction. Through 5mm incisions, specialised instruments (such as irrigated burrs) are used under x-ray guidance to re-align and stabilise the bones and joints.
Advantages include:
- Tiny incisions
- Less postoperative great toe stiffness
- Minimal scarring
- Reduced discomfort
- Quicker recovery
- Less infection risk.
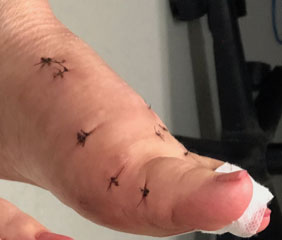
Small incisions used for minimally invasive bunion surgery
There are certain cases where minimally invasive surgery for Bunion correction may not suitable for your foot. In this situation, Mr Goldbloom will discuss other surgical options such as:
- Scarf osteotomies
- Corrective fusions
- Soft tissue releases.
Post-operative Care
- Patients usually weight-bear in a stiff sole open toe shoe from day one. You will be seen by a Physiotherapist whilst in hospital who will provide you with the appropriate footwear and ensure you are able to manage your post-operative weight-bearing instructions. A Physiotherapist will be involved post-operatively to help you regain range of motion of the big toe and to help with swelling control.
- You will have a wound review 2-3 weeks with Mr Goldbloom and a Wound Nurse Specialist.Your dressings are to stay dry and intact until this appointment.
- You will have an appointment with Mr Goldbloom 6 weeks after your surgery with an updated weight-bearing x-ray to assess alignment and healing. It will be decided at this appointment if it is safe for you to wear normal footwear.
- When you go home it is very important to elevate the foot 23 hours a day above the level of your heart for two weeks.
Refer to the Foot and Ankle Surgery information sheet for further post-operative instructions.
Exercises after Bunion Surgery
This video is a collaboration with the Principal Physiotherapist and Head of Strength and Conditioning at the Australian Ballet. They developed this program for their dancers who as a result have a much lower injury rate in their feet.
These exercises also apply to my patients undergoing rehab after bunion surgery, bunionette surgery or 2nd toe surgery. Note, this video does not apply to great toe fusion surgery.
Rehabilitation Plan
On your mobile? Click the green + to see the full instructions for each week
| Week | Exercises | Boot | Weight bearing | Returning to Pre-Surgical Function | Other |
|---|---|---|---|---|---|
| 0-2 | Ankle circles Foot and lower leg massage. | Post-op shoe | Weight bearing as tolerated | Staying home with the foot elevated above heart level for 23 hours a day | |
| 2-4 | Light ROM “fairy fingers” for dorsiflexion and plantarflexion exercises. Seated low force toe raises and heel raises. Working towards 30 mins walking. | Post-op shoe | Weight bearing as tolerated | Never pushing the joint to end ROM- no sprinting off blocks or extreme DF for 12/12 | |
| 4-6 | Calf stretching. Physio guided 1st toe mobilisations Hip, knee, ankle band resisted exercises. Resisted seated heel and toe raises, feet tapping, short foot and arch lift exercises. Continue exercises a/a. Start DL heel raises, progressing to SL. | Full weight bearing | Return to work – sedentary occupation. | ||
| 6-8 | Patient guided 1st toe flex and ext mobilisations, toe ball squeeze, toe squeeze and spread. Physio guided gait and balance training | Walking as tolerated. Return to light duties – labour intensive occupation | |||
| 8-10** | Increase walking distance. Progress exercises a/a with physio guidance | ||||
| 10-12* | Physio guided, gradual return to pre-surgery activities eg. running, cycling. | ||||
| 12+ | Return to sport training for higher level functioning patients. |
If you have any questions please do not hesitate to contact Mr Goldbloom’s rooms on 03 9650 0534.
This rehabilitation plan was developed by Mr Goldbloom in conjunction with Physiotherapists Brodie Leonard-Shannon and Brendan Mason from Back in Motion, Aspendale Gardens.
The information provided here is for general educational purposes only. Please contact Mr Goldbloom's rooms to discuss if surgery is appropriate for your situation.

