Plantar Fasciitis
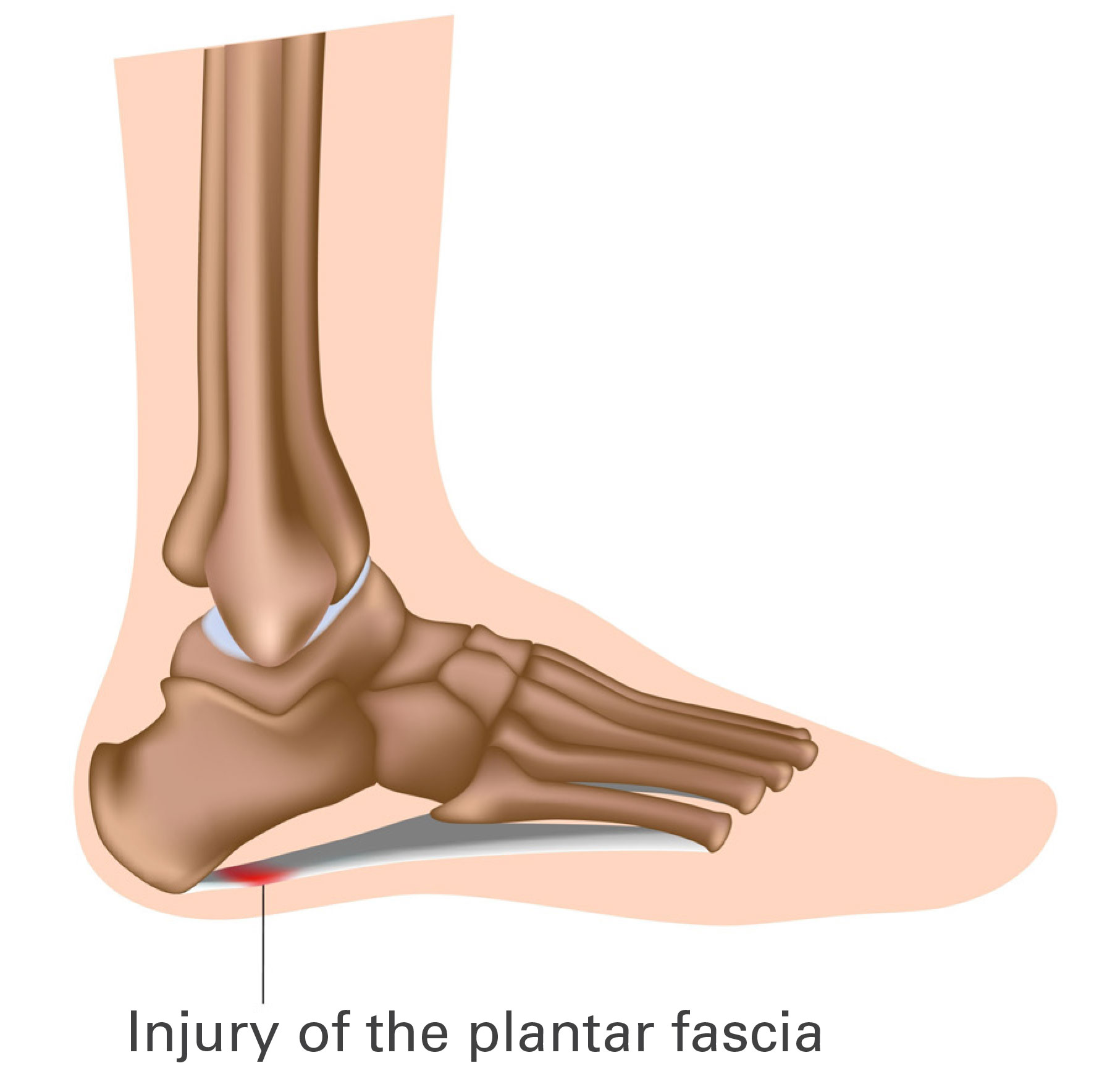
The Plantar Fascia is a fibrous sheet of tissue that attaches at the heel bone (calcaneus) extending along the sole all the way to the toes. It helps to hold the arch of your foot.
Plantar Fasciitis occurs when this attachment is “stressed” more than usual which leads to damage of that part of the Plantar Fascia.
Risk factors include:
- Repetitive stress exercise such as in long-distance runners
- Weight gain
- New footwear
- Jobs that involve standing for long hours on hard floor.
Symptoms
Patients experience pain on the sole of the foot, usually near the heel bone but often extending into the arch of the foot. Classically, it is painful when you first put your foot to the floor in the morning. The pain is often made worse by long periods of standing and walking.
What Imaging is Needed?
You may be asked to obtain a Magnetic Resonance Imaging (MRI) scan to assess the injury to the Plantar Fascia and make sure there is no stress reaction in the heel bone.
Non-Surgical Treatment
In a high percentage of cases, symptoms go away with non-surgical treatment, but this can take two years.
Non-surgical treatment will initially involve:
Footwear modification prescribed by your Podiatrist. This may include the use of a gel heel pad to cushion the painful area. A heel raise will shorten the calf length slightly which reduces the stretch on the injured area.
An exercise plan put together by your Podiatrist or Physiotherapist. This may include “Plantar Fascia Specific Stretching” which involves rolling the painful area over cold or roughened surfaces. “Heel cord stretching” is aimed at stretching the calf muscles which in turn reduces the stress under the heel. Taping techniques may also be incorporated into your exercise plan.
Other non-surgical options include:
- A Night Splint that holds the ankle at 90 degrees. This will keep the calf stretched out at night to prevent that initial pain in the morning.
- Shock Wave Therapy involves pulses of ultrasound that will encourage healing.
- Steroid Injection may relieve your pain but carries a risk of further damage to the Plantar Fascia.
- Blood Injection (platelet rich plasma) aids the healing process by giving a high concentration your own blood, and its associated healing properties, directly to the injured area.
Surgical Treatment
Surgery is reserved for cases where the non-surgical options have failed. A successful outcome may not be evident for a few months.
Mr Goldbloom performs two surgeries for Plantar Fasciitis. These options and specific risks to each surgery will be discussed at your consultation.
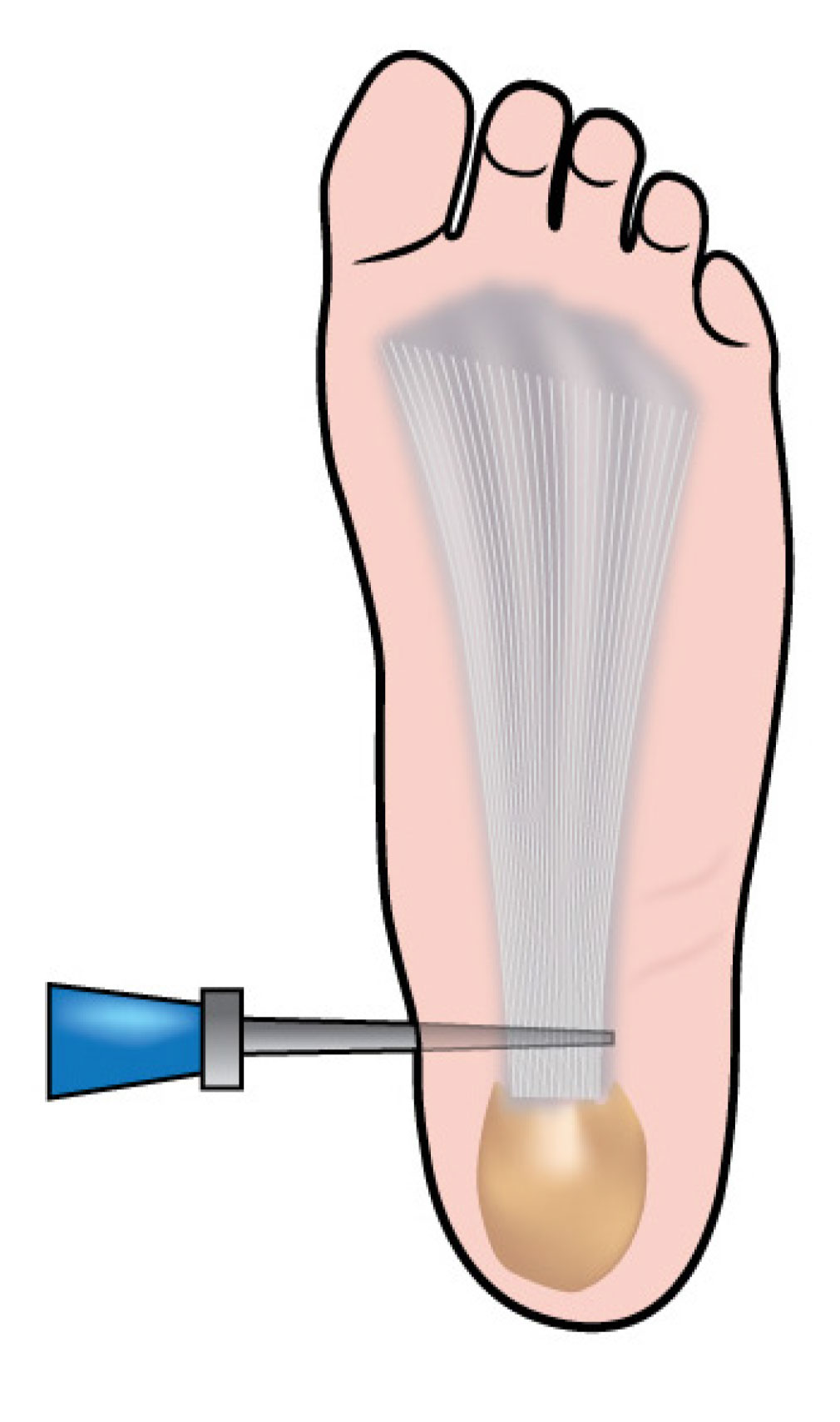
Plantar Fascia Release is a common procedure and can be performed using two different techniques.
Keyhole type surgery is one technique that can be used and is performed using a small incision near the attachment of the Plantar Fascia to the heel bone.
In certain instances however, a nerve known as a Baxter’s nerve is irritated by the Plantar Fasciitis, and an open procedure will need be performed to ‘free’ the nerve in addition to the Plantar Fascia release.
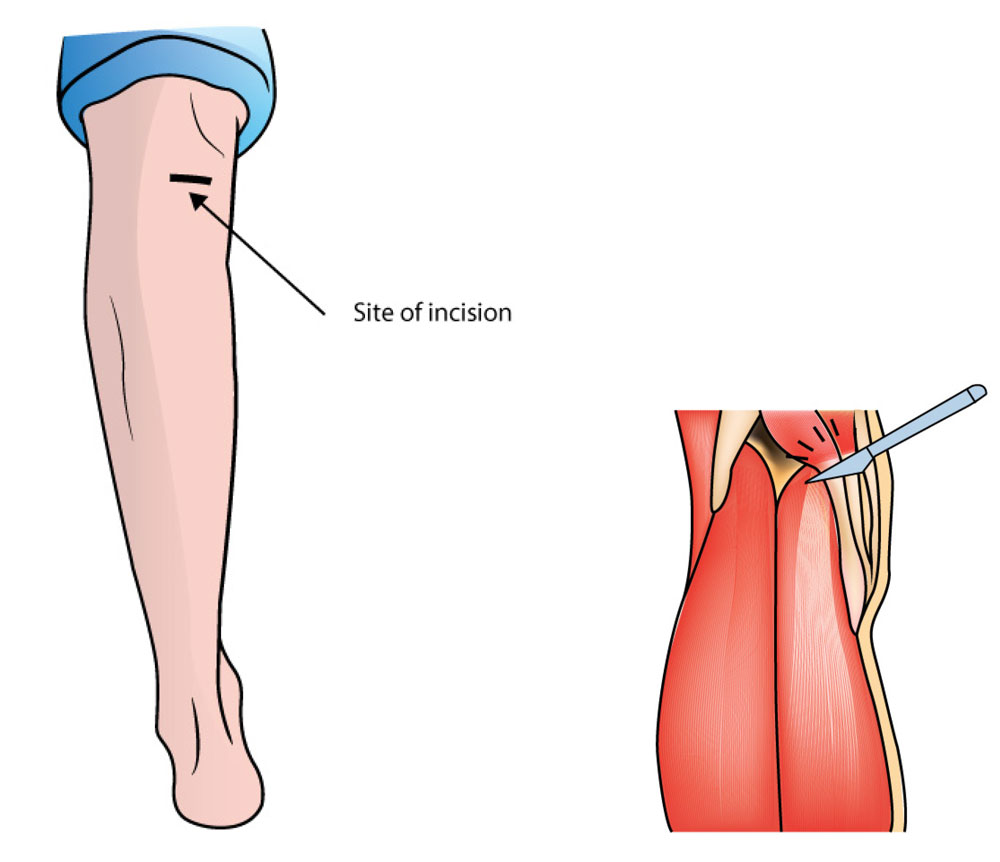
Proximal Medial Gastrocnemius Release is performed by a small incision high up on the calf just below the back of the knee.
It is an indirect technique to reduce the stress on the injured Plantar Fascia allowing it time to heal.
It has the advantage of a fast recovery and avoids risks associated with surgery near the sole of the foot.
Post-operative Care for Plantar Fascia Release
- When you go home it is very important to elevate the foot 23 hours a day above the level of your heart for two weeks.
- You will be required to non-weight bear for 2 weeks.
- You will have a consultation with Mr Goldbloom and the Wound Nurse Specialist approximately 2-3 weeks after your surgery. Leave your dressings intact until this review.
- Physiotherapy will be required post-operatively. It will be tailored to you and how well you are recovering.
Refer to the Foot and Ankle Surgery information sheet for further post-operative instructions.
Rehab Protocol for Endoscopic Plantar Fascial Release
On your mobile? Click the green + to see the full instructions for each week
| Week | Exercises | Boot | Weight bearing | Returning to Pre-Surgical Function |
|---|---|---|---|---|
| 0-2 | Toe wriggling Ankle circles Hip and knee band resisted exercises. | Shoes with arch support (ie. runners) all the time | TWB | Staying home with the foot elevated above heart level for 23 hours a day |
| 2-4 | Band resisted ankle DF/PF, in/eversion. Seated CRs, feet tapping. | Shoes with arch support (ie. runners) all the time | WBAT | |
| 4-6 | Short foot and arch lift exercises. Elevated DL heel raises progressing to floor | Shoes with arch support (ie. runners) all the time | WBAT/FWB | |
| 6-8 | Toe lifts, bends, pulls, pushes, toe ball squeeze, toe squeeze and spread. Physio guided gait and balance training | Normal flat shoes 50% of the time. | FWB | |
| 8-10** | Increase walking distance. | Any footwear | FWB | |
| 10-12* | Physio guided, gradual return to pre-surgery activities eg. running, cycling. | FWB | ||
| 12+ | Return to sport training | FWB |
Post-operative Care for Proximal Gastrocnemius Release
- You can weight bear as tolerated after your operation and rest as much as possible for 2 weeks.
- You will have a consultation with Mr Goldbloom and the Wound Nurse Specialist approximately 2-3 weeks after your surgery. Leave your dressings intact until this review.
- Physiotherapy will be required post-operatively. It will be tailored to you and how well you are recovering.
Refer to the Foot and Ankle Surgery information sheet for further post-operative instructions.
The information provided here is for general educational purposes only. Please contact Mr Goldbloom's rooms to discuss if surgery is appropriate for your situation.
